
Blog
-
Skin Care Tips for a Radiant Complexion
posted: Aug. 14, 2023.

-
The Power of Chemical Peels
posted: Aug. 01, 2023.

-
Understanding Acne: Causes and Treatment Options
posted: Jul. 13, 2023.

-
Treating Eczema in Adults
posted: Jul. 01, 2023.
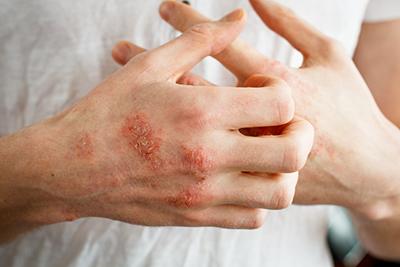
-
Common Causes of Rashes
posted: Jun. 21, 2023.
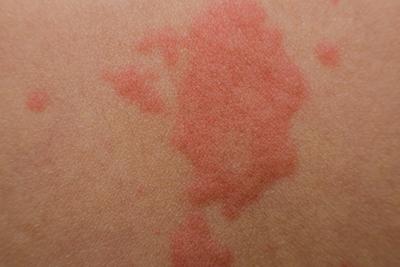
-
Treatment Options for Acne Scarring
posted: Jun. 06, 2023.
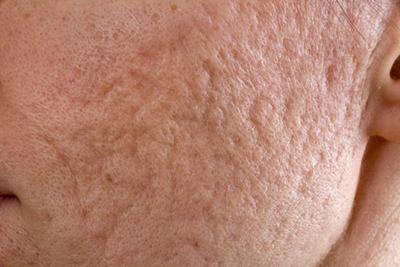
-
The ABCDEs of Skin Cancer: Understanding the Signs and Symptoms
posted: May 15, 2023.
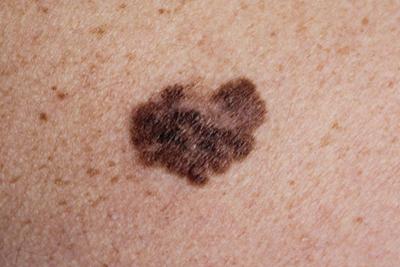
-
Eczema: Understanding Triggers and Treatment Options
posted: May 08, 2023.
-
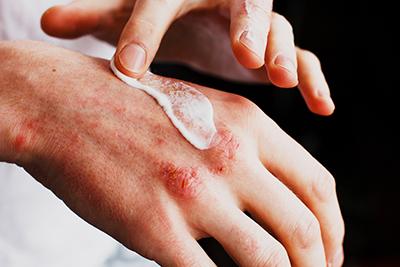
Common Skin Conditions: Eczema, Psoriasis, and Rosacea Explained
posted: Apr. 21, 2023.

-
Skin Cancer Prevention Tips
posted: Apr. 07, 2023.

-
Skincare Tips for Every Skin Type: How to Keep Your Skin Healthy and Radiant
posted: Mar. 23, 2023.

-
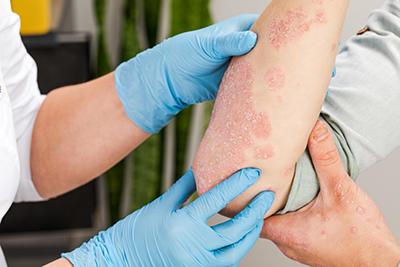
Understanding Common Skin Conditions and How to Manage Them
posted: Mar. 10, 2023.
-
Understanding and Managing Acne
posted: Feb. 27, 2023.

-
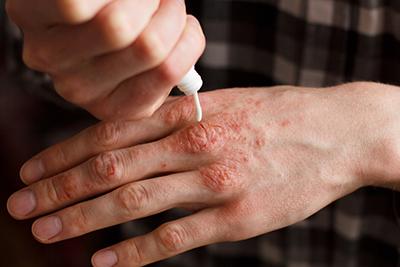
How to Treat and Prevent Eczema Flare-Ups
posted: Feb. 07, 2023.
-
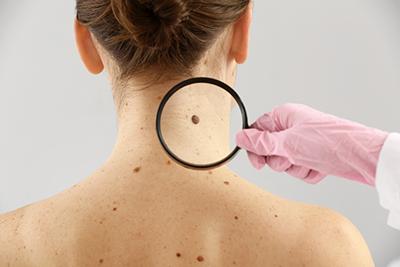
The Benefits of Regular Skin Cancer Screenings
posted: Jan. 25, 2023.
-
Non-Invasive Anti-Aging Treatments
posted: Jan. 11, 2023.
There are many factors which can combine to make you look older than you are. Sun exposure, harmful chemicals or cosmetics, bad diet, lack of hydration, and the accumulation of Read more